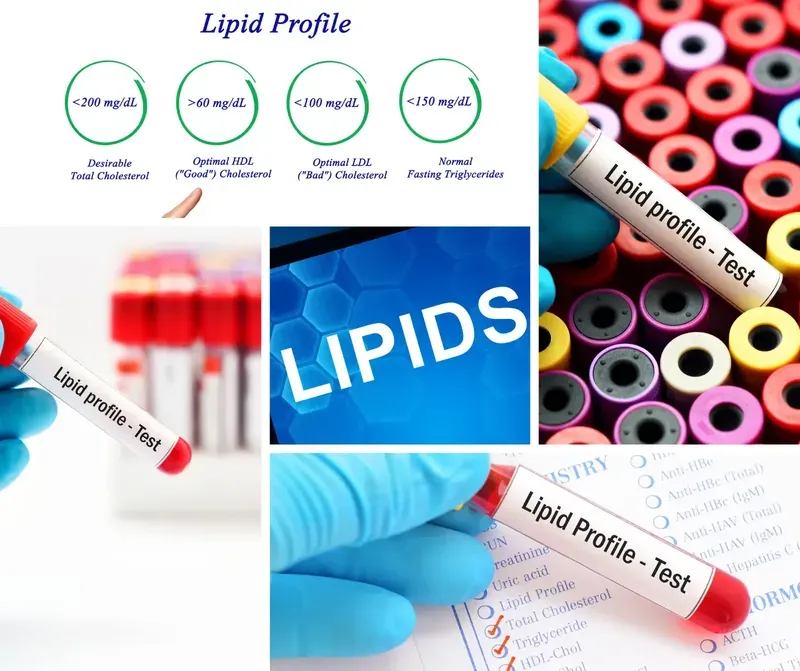
What is the lipid profile test used for?
A lipid profile measures the levels of cholesterol and other fats in your blood. It is used to screen for, diagnose, and monitor heart disease and other health conditions.
The main types of cholesterol are high-density lipoprotein (HDL), low-density lipoprotein (LDL), and very-low-density lipoprotein (VLDL). HDL is often called "good" cholesterol because it helps keep the bad cholesterol from building up in your arteries. LDL is often called "bad" cholesterol because it can clog your arteries.
Your doctor may order a lipid profile if you have risk factors for heart disease, such as high blood pressure, diabetes, or a family history of heart disease.
Lipid levels are important because they give a measure of the risk of developing cardiovascular disease. The lipid profile measures the levels of cholesterol and triglycerides in the blood.
Cholesterol is a type of fat that is found in all cells in the body. It is used to make hormones, Vitamin D, and substances that help you digest food. There are two types of cholesterol - HDL (high-density lipoprotein) and LDL (low-density lipoprotein). HDL is sometimes called "good" cholesterol because it helps to remove bad cholesterol from the blood. LDL is sometimes called "bad" cholesterol because it can build up on the walls of arteries and increase your risk for heart disease.
There are a variety of blood tests that can be used to assess your lipid profile. The most common lipid panel measures total cholesterol, low-density lipoprotein (LDL) cholesterol, high-density lipoprotein (HDL) cholesterol, and triglycerides.
Having high levels of total cholesterol and LDL cholesterol puts you at risk for heart disease. HDL cholesterol helps protect against heart disease, so it's important to have high levels of HDL cholesterol. Triglycerides are a type of fat in the blood that can increase your risk for heart disease if they're too high.
A lipid profile measures the levels of cholesterol and other fats in your blood. These tests can help you and your doctor understand your risk for heart disease. The American Heart Association (AHA) recommends that all adults aged 20 years or older have a lipid profile done at least every 5 years.
There are several types of blood tests that can measure cholesterol levels. The most common test measures total cholesterol, HDL cholesterol, LDL cholesterol, and triglycerides. Your doctor may also order a VLDL (very low-density lipoprotein) test to measure the amount of VLDL cholesterol in your blood. This type of test is not as common as the other tests, but it may be ordered if you have a high triglyceride.
A lipid profile measures different types of cholesterol and triglycerides in your blood. Cholesterol and triglycerides are "lipids", which are a type of fat. Lipids are important for the body because they help you to store energy, and they are also necessary for the production of hormones.
There are two types of cholesterol - HDL (high-density lipoprotein) and LDL (low-density lipoprotein). HDL is often called the "good" cholesterol because it helps to remove LDL from the blood. LDL is often called the "bad" cholesterol because it can build up in the arteries and cause them to become blocked.
Triglycerides are another type of lipid that can be increased by eating too many
A lipid profile measures the levels of various fats and cholesterol in your blood. It can help determine your risk for heart disease and other health problems. The test typically includes a measure of total cholesterol, HDL cholesterol, LDL cholesterol, and triglycerides
Your doctor may recommend a lipid profile if you have risk factors for heart disease, such as high blood pressure, high blood sugar, or a family history of heart disease. The test can also help monitor your treatment if you have been diagnosed with heart disease.
A lipid profile measures the various types of cholesterol and triglycerides in your blood. The main purpose of a lipid profile is to see if you have high levels of low-density lipoprotein (LDL) cholesterol, which is known as the "bad" cholesterol because it can deposit in your arteries and increase your risk of heart attack and stroke. A lipid profile can also give you a measure of your high-density lipoprotein (HDL) cholesterol, which is known as the "good" cholesterol because it helps remove LDL cholesterol from your arteries. A lipid profile may also provide information about the levels of triglycerides in your blood, which are a type of fat that can contribute to heart disease
Lipid profile blood tests measure levels of lipids in your blood. Lipids are a type of molecule that includes cholesterol, triglycerides, and phospholipids. Your lipid profile can give your doctor important information about your risk for heart disease. Your doctor may use your lipid profile to help make decisions about treatment and prevention strategies for you. A lipid profile measures the levels of fats (lipids) in your blood. It is important to know your lipid levels because they can indicate your risk for heart disease.
There are four primary types of lipids that are measured in a lipid profile: total cholesterol, HDL cholesterol, LDL cholesterol, and triglycerides. Your doctor will use these measurements to calculate a number known as your "total cholesterol to HDL ratio". This number is used to determine your risk for heart disease.
If you have high total cholesterol or LDL cholesterol levels, or high triglyceride levels, you are at increased risk for heart disease. If you have low HDL cholesterol levels, you are also at increased risk for heart disease.
Blood tests for lipid profile usually include total cholesterol, HDL cholesterol, LDL cholesterol, and triglycerides. They can help to identify whether someone is at risk for heart disease.
HDL cholesterol is known as the "good" type of cholesterol because it helps to remove bad cholesterol from the blood. LDL cholesterol is known as the "bad" type of cholesterol because it can buildup on the walls of arteries and cause heart disease. Triglycerides are a type of fat that is carried in the blood. A high level of triglycerides can increase the risk of heart disease.