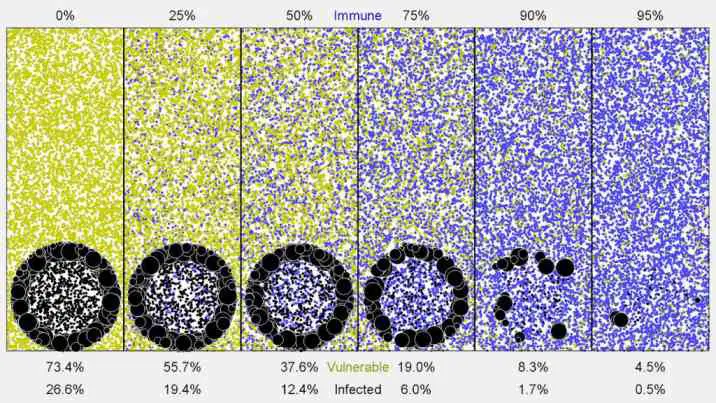
Herd immunity: the basics
Many countries have been in lockdown for over a month, and some have tried to begin the discussion of an exit strategy. We know that remaining in lockdown continuously is not a feasible strategy, as many people have been suffering economic consequences from the stringent lockdown measures, and many countries have been providing significant monetary and fiscal support for people and businesses at risk. But leaving lockdown too early has its own consequences.
Almost all public health professionals will agree that the lockdown has been able to significantly reduce infection rates and reduce the pressure on our healthcare systems. By taking this early victory and prematurely ending lockdown we risk another wave of infections, reintroducing lockdown, and having an overall negative effect on the general health of the populous.
So what can we do? One exit strategy that has been touted recently is herd immunity. To understand how to may work for COVID we must understand what epidemiologists mean by herd immunity.
IMMUNITY
Our body’s immune system fights against invading organisms such as bacteria and viruses. For a more in-depth discussion you can have a look at previous blogs on Vaccines and Boosting the Immune system. The immune system is very competent and has mechanisms to theoretically recognise any protein tags that do not belong to that person’s cells, even protein tags that do not currently exist in nature. This gives the immune system the ability to theoretically recognise nearly any invading organism that has existed or will ever exist.
The immune system goes beyond this as well and produces “memory cells”. These remain in the blood after an infection for a long time; in some cases, it can even be lifelong. When a second infection occurs from the same organism the immune system jumps into action and is able to produce antibodies against the invader almost immediately. This can neutralise the invader before it has a chance to replicate, cause severe symptoms and harm the body. Sometimes we never realise we have been infected as the infection never gets a chance to cause any damage.
Importantly, if the invader cannot replicate in our body, then its ability to spread to other people is also reduced. For example, respiratory viruses can rapidly replicate in our lungs and be transmitted when we cough or sneeze. By eliminating the virus before it can replicate extensively the number of viral particles in each cough and sneeze is reduced, reducing the chances of another person catching the infection.
This is the basis of how vaccines work and is covered in depth in the two part blog.
HERD IMMUNITY
If our immune system is so competent, why do we need to worry about infections at all? Surely we can all get infected and gain immunity. In an ideal world where everyone was healthy this may be true. But there are many people who do not have fully functioning immune systems. These people are immunocompromised and can be for many reasons.
- Chemotherapy and radiotherapy for cancer destroys rapidly dividing cells such as cancer cells. Unfortunately, it also hits other dividing cells, such as hair follicles, gut lining and the bone marrow, which produce the white blood cells that give us immunity. Chemotherapy patients are very susceptible to even the mildest of infections. Even if a mild infection is suspected, they are treated aggressively with antibiotics, as their lowered immune systems can become overwhelmed very quickly.
- Sometimes doctors advise patients to take medication that purposefully dampens the immune system. This is necessary for transplant patients, where the host immune system attacks the donor organ as it does not belong to the host, or in autoimmune disorders, where the immune system attacks the host by mistakenly recognising it as an “invader”.
- Taking steroids long term has a similar effect, and is used quite commonly for skin disorders, asthma, COPD, and other inflammatory conditions.
- People with various chronic illnesses can have reduced immunity as a result of the illness. High sugar levels associated with poorly controlled diabetes can cause worsening organ function, including the immune system. These patients are more susceptible to infections.
- Finally, some people do not have fully functioning or welldeveloped immune systems for a variety of reasons, inherited or acquired. As we get older, the immune system function decreases, and simple infections can be devastating.
In all of these cases the ability to recognise invading organisms, destroy them and form immunity is hampered. Vaccination, one way of inducing immunity without causing the person to suffer from a full-blown infection, can also be ineffective in these patients, and some vaccines can be dangerous if used incorrectly. So how do we protect these vulnerable patients?
HERD IMMUNITY
This is where we go back to the earlier point. Immunity in healthy people can reduce or even prevent the spread of infection from one person to another. The number of healthy people outnumber the number of vulnerable, immunocompromised ones. Therefore, if we induce immunity in most people, the infection will simply not spread to the vulnerable ones. We don’t have to immunise everyone, just enough to prevent transmission. This is called herd immunity. This is why we immunise everyone with flu vaccines even those that are healthy and will survive a full blown infection. Because by preventing these people from inadvertently spreading the flu, they will protect those that we cannot immunise.
Does herd immunity work? For most other diseases, yes. It depends on how the disease is spread, and how infective it is. For measles, you need to immunise 19 out of 20 people to achieve herd immunity, because it is so infective. But once herd immunity was achieved death rates were drastically reduced. With the advent of anti-vaccine campaigns, particularly against MMR, this herd immunity has been lost, and many vulnerable children (and adults) who do not have fully functioning immune systems are now contracting this virus and dying from a preventable disease.
It can be achieved for pandemics as well. Norway was able to achieve partial herd immunity to H1N1 (swine flu) through a vaccination program and natural immunity. Vaccines are the best method for achieving herd immunity without extremely high death rates. We have already covered the issues with making a vaccine, and why it takes such a long time, in our previous blog
From reading this blog you should now have an understanding of what herd immunity is, and why it is important in protecting those that are vulnerable to infections. In our next blog we will look at why herd immunity may not be the solution for COVID-19.
Dr Rajan Choudhary, UK, Chief Product Officer, Second Medic Inc
www.secondmedic.com