Crohn’s disease is a chronic inflammatory condition that primarily affects the gastrointestinal (GI) tract. As part of inflammatory bowel disease (IBD), Crohn’s disease can lead to significant discomfort and complications if left untreated. Understanding its causes, symptoms, and manifestations is crucial for effective diagnosis and management.
The Basics of Crohn’s Disease
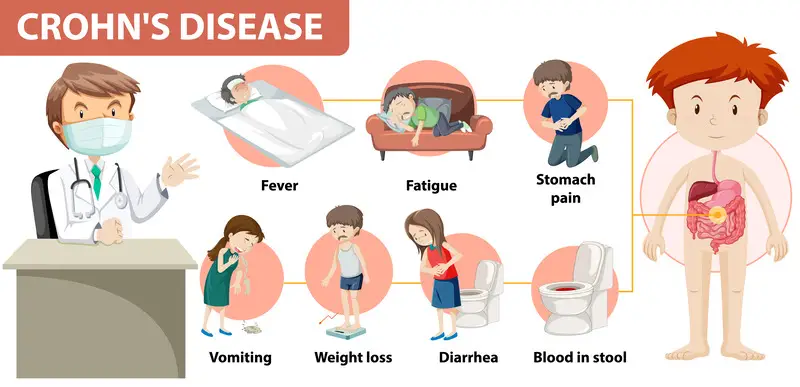
Crohn’s disease can affect any part of the GI tract, from the mouth to the anus. Common Crohn’s disease symptoms include abdominal pain, diarrhoea, fatigue, weight loss, and malnutrition. However, its causes remain multifactorial and involve a complex interplay of genetic, environmental, and immune-related factors.
Genetic Causes of Crohn’s Disease
Research shows a strong genetic predisposition in individuals with Crohn’s disease. If a close relative, such as a parent or sibling, has Crohn’s, your risk of developing the condition increases significantly. Scientists have identified several gene mutations linked to Crohn’s, particularly those affecting immune system regulation.
The NOD2 gene is one example. Mutations in this gene can impair the immune response to gut bacteria, increasing inflammation in the intestines. Recognizing the genetic causes of Crohn’s disease not only helps in early diagnosis but also provides insight into tailored treatments targeting these pathways.
Causes of Crohn’s Disease in Young Adults
Crohn’s disease often manifests in individuals between the ages of 15 and 35, though it can occur at any age. In young adults, hormonal changes, lifestyle factors, and stress may exacerbate the risk of disease onset. For those with undiagnosed Crohn’s disease symptoms, this stage of life is particularly critical, as symptoms may overlap with other conditions like irritable bowel syndrome (IBS).
Young adults may experience more severe Crohn’s disease symptoms, including abdominal cramping and persistent diarrhoea. Early intervention through a Crohn’s disease symptoms test can prevent long-term complications.
Environmental Factors in Crohn’s Disease
The role of the environment cannot be overlooked. Factors such as diet, exposure to pollutants, and urban living have been associated with increased Crohn’s prevalence. Diets high in processed foods and low in fibre may disrupt gut microbiota, leading to inflammation.
In addition, antibiotics, while often necessary, can alter gut bacteria and potentially trigger flare-ups. Recognizing these environmental factors in Crohn’s disease can empower patients to adopt preventive measures like balanced diets and mindful antibiotic use.
Autoimmune Link in Crohn’s Disease
Crohn’s disease is widely considered an autoimmune or autoinflammatory condition. The immune system mistakenly attacks the healthy tissues of the GI tract, leading to chronic inflammation. Dysregulation in immune signalling pathways is central to Crohn’s disease manifestations.
Autoimmune diseases often cluster, so individuals with other autoimmune disorders like rheumatoid arthritis or psoriasis may have a heightened risk. Understanding the autoimmune link in Crohn’s disease helps identify at-risk individuals and develop effective treatment protocols.
How Smoking Impacts Crohn’s Disease
Smoking is a well-established risk factor for Crohn’s disease. Smokers are twice as likely to develop the condition compared to non-smokers. Moreover, smoking can worsen symptoms and reduce the efficacy of certain treatments.
Nicotine and other chemicals in cigarettes may alter immune function and gut flora, contributing to inflammation. Smoking cessation is one of the simplest yet most impactful ways to improve outcomes in individuals with Crohn’s.
Diagnosing Crohn’s Disease
Diagnosing Crohn’s disease can be challenging due to the variability of its symptoms. A combination of tests, including:
-
Blood tests to detect inflammation or anaemia
-
Stool teststo rule out infections -
Endoscopic procedures like colonoscopy
-
Imaging studies like MRI or CT scans
These tools are essential for confirming undiagnosed Crohn’s disease symptoms and ruling out other potential causes.
Treatment Approaches for Crohn’s Disease
Though there is no cure, Crohn’s disease treatment focuses on reducing inflammation, managing symptoms, and preventing complications. Treatment options include:
-
Medications: Anti-inflammatory drugs, immunosuppressants, and biologics targeting specific immune pathways.
-
Dietary Adjustments: Avoiding trigger foods and incorporating anti-inflammatory diets.
-
Surgery: Reserved for severe cases involving intestinal blockages or fistulas.
-
Lifestyle Modifications: Stress management, smoking cessation, and regular exercise.
Crohn’s Disease Manifestations Beyond the Gut
While primarily a gastrointestinal condition, Crohn’s disease can affect other parts of the body. Common extra-intestinal manifestations include:
-
Joint pain and arthritis
-
Eye inflammation
-
Skin conditions like erythema nodosum
-
Delayed growth in children
Addressing these Crohn’s disease manifestations often requires a multidisciplinary approach.
Second Medic’s Role in Crohn’s Disease Management
At Second Medic, we offer a comprehensive range of diagnostic and management services for Crohn’s disease. From conducting advanced Crohn’s disease symptom tests to providing personalized treatment plans, our team of specialists ensures holistic care. Additionally, we prioritize patient education, empowering you to manage your condition effectively.
Final Thoughts
Understanding the causes of Crohn’s disease is the first step toward effective management. Whether it’s genetic predisposition, environmental triggers, or immune dysfunction, identifying the root cause helps in tailoring treatments. If you’re experiencing Crohn’s disease symptoms, seek timely medical advice to prevent complications and enhance your quality of life.
For expert guidance and testing, connect with Second Medic today. Let us help you navigate your journey to better health.