TREATING COVID WITH BLOOD
We have previously covered proposed treatments for COVID-19, in particular hydroxychloroquine, and explained why we shouldn’t look for a magic cure for this disease. Viruses are difficult to treat, and ultimately supportive treatment appears to be best we can achieve. But an editorial published in BioMedicine Central appears to show a novel treatment for the most ill patients, one that may have flown under most people’s radar.
“A novel treatment approach to the novel coronavirus: an argument for the use of therapeutic plasma exchange for fulminant COVID-19”
An interesting title. Lets dissect it.
SUMMARY
- Blood is made up of many different components
- The immune system recognises the virus and produces antibodies against it to neutralise it
- These antibodies float in the blood plasma, a watery solution
- The plasma can be extracted from donated blood, and given to patients suffering from COVID-19
- So far evidence suggests it can help treat the most seriously affected patients.
WHAT IS IN OUR BLOOD
To understand this we must first understand what our blood is made of. Most people know that blood functions to transport oxygen from our lungs. But this is an oversimplification. Blood has many different functions:
- Transport: along with oxygen it transports sugars, fats, protein subunits throughout the body. This is done with the watery PLASMA of the blood.
- Clot: cells and protein structures act to plug any holes that form from cuts and damage. This is done by the PLATELETS in the blood
- Immunity: Immune cells respond to bacteria, viruses, parasites in the blood and body. They target these pathogens, identify and tag them with antibodies, and ultimately destroy them. This is done by the WHITE BLOOD CELLS.
And many more functions that we won’t bore you with.
IMMUNITY
It is this last point that is of interest to us. Our immune system consists of white blood cells that can recognise invading organisms in the blood, around cells and even invaders hiding within our own cells. All cells have protein markers on their surface, no matter if its human cells, bacterial, viral, fungal etc. These markers can be highlighted and targeted by specialised white blood cells, who in turn produce antibodies against these markers. Think of antibodies as handcuffs with flares attached: once attached other white blood cells use this information to find and destroy the invaders.
What is amazing about antibodies is how complex they are. The proteins in our body are incredibly complex. They are long chains that fold into unique shapes depending on hundreds of different types of chemical interactions. These are so complex that supercomputers can take literal years to figure out the shape of a single protein and how it folds depending on the subunits in its chain. This means that our immune system has to recognise these markers and figure out a complementary tag out of hundreds of billions of potential sequences. Antibodies have to be specific to their tag. If an antibody is produced that can target more than one tag, it can cause problems. If it targets a bacterial tag, but accidentally highlights the person’s cells as well, the immune system will start targeting and destroying the person’s organs. These auto-immune disorders can be devastating.
But when they work, antibodies are miraculous. They persist in the blood after an infection, and if a second infection occurs, memory cells in the blood can rapidly produce these antibodies before the infection can even produce symptoms. This is known as immunity, and is why we usually don’t get the same illness twice. Antibody based treatment is see as the future of medical therapy, and is something we will cover in future blogs.
PLASMA EXCHANGE
From population testing we can see that the majority of patients with COVID-19 recover, experiencing either mild symptoms, moderate symptoms requiring some form of treatment and hospitalisation, or no symptoms whatsoever. In these patients their immune system will have successfully recognised the virus and produced antibodies against it to neutralise the virus. It is the patients with severe symptoms, those in which the virus is running rampant in the body, that the production of antibodies happens too late.
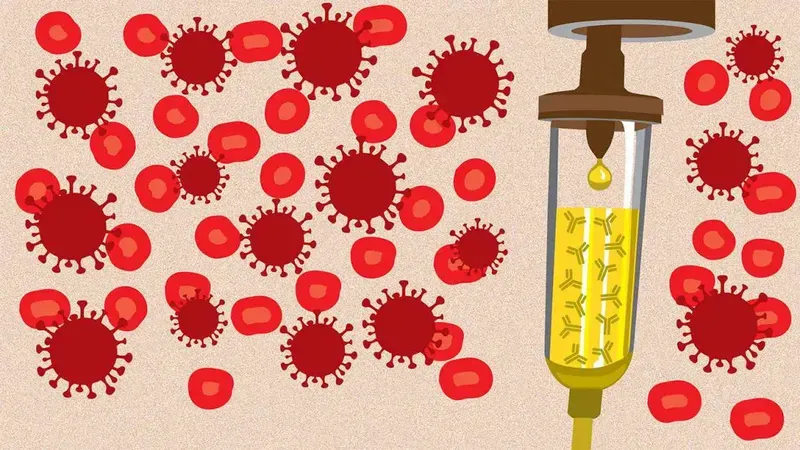
Plasma exchange involves obtaining blood from patients who have beaten the virus, spinning the blood to separate out the red cells, white cells, platelets and watery plasma. The plasma contains all the glucose, small proteins and importantly for us, the antibodies. This plasma can be transfused into patients with COVID-19 that cannot cope, in order to help their immune system. These transfused antibodies will neutralise some of the viruses in the patient, reducing the viral load, amount of replication and cell destruction that causes such devastating symptoms in COVID-19.
The published editorial showed that in the most critical pneumonia patients, requiring mechanical ventilators and drugs to support the heart, mortality in plasma exchange patients resulted in a 47.8% mortality instead of 81.3%. Of course it is a single study with a limited number of patients, but the results are encouraging. It is further helped by the fact plasma exchange is a well established therapy, with established protocols known to intensivists and haematologists.
THE FUTURE
We may see the use of Plasma exchange for critically ill patients increase as the pandemic continues. It is not a treatment option available for everyone, as it requires intravenous access and careful monitoring in a controlled setting. But it also needs donation from people who have recovered from COVID and have suitable antibodies. So whilst it might not be a magic pill that everyone expects to cure COVID, it might be the difference between life and death for those that need it most.
Dr Rajan Choudhary, UK, Chief Product Officer, Second Medic Inc