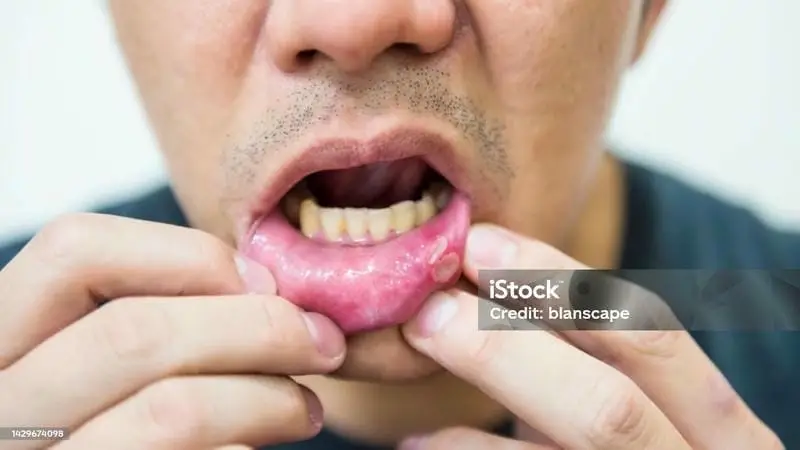
Mouth ulcers are small, painful sores that appear inside the mouth, on the tongue or along the gums. While an occasional ulcer is common and usually harmless, many people experience ulcers repeatedly. Understanding the causes of frequent mouth ulcers is important because recurrent ulcers often signal underlying health or nutritional issues rather than a simple oral problem.
In India, recurrent mouth ulcers are commonly linked to dietary deficiencies, stress and digestive health issues.
What Are Mouth Ulcers?
Mouth ulcers, also known as aphthous ulcers, are shallow sores with:
-
a white or yellow centre
-
red, inflamed borders
They are not contagious but can cause significant discomfort while eating or speaking.
Why Do Mouth Ulcers Become Frequent?
Frequent ulcers indicate that the mouth lining is not healing properly or is repeatedly exposed to triggers.
This can happen due to:
-
nutritional deficiencies
-
immune system imbalance
-
chronic stress
-
underlying medical conditions
Nutritional Deficiencies: The Most Common Cause
Vitamin B12 Deficiency
Vitamin B12 is essential for cell repair and nerve health.
Deficiency can cause:
-
recurrent mouth ulcers
-
burning tongue
-
fatigue
NFHS-5 data shows widespread micronutrient deficiencies in India.
Iron Deficiency
Iron deficiency reduces oxygen supply to tissues.
This leads to:
-
delayed healing
-
frequent oral sores
-
pale oral lining
Iron-deficiency anemia is a major contributor to oral ulcers.
Folate Deficiency
Folate supports cell turnover.
Low folate levels impair regeneration of the mouth lining, increasing ulcer risk.
Stress and Psychological Factors
Stress is a well-recognised trigger.
Chronic stress:
-
suppresses immune function
-
increases inflammation
-
delays wound healing
WHO mental health studies highlight stress as a major contributor to recurrent oral ulcers.
Immune System Imbalance
The immune system plays a critical role in oral health.
Frequent mouth ulcers may occur due to:
-
autoimmune tendencies
-
immune hypersensitivity
-
chronic inflammation
Some ulcers form due to the immune system attacking oral tissues.
Digestive and Gut Health Disorders
Digestive health is closely linked to oral health.
Conditions associated with frequent ulcers include:
-
acidity and gastritis
-
inflammatory bowel disease
-
malabsorption syndromes
Poor nutrient absorption worsens deficiencies and ulcer recurrence.
Hormonal Factors
Hormonal fluctuations can trigger mouth ulcers.
Common situations include:
-
menstruation
-
pregnancy
-
hormonal disorders
Women may notice ulcers recurring at specific times in the menstrual cycle.
Food Sensitivities and Irritants
Certain foods irritate the oral lining.
Common triggers include:
-
spicy foods
-
acidic fruits
-
nuts
-
chocolate
Repeated exposure increases ulcer frequency.
Oral Trauma and Habits
Minor injuries can initiate ulcers.
These include:
-
accidental cheek biting
-
sharp teeth or braces
-
aggressive brushing
Poor oral hygiene delays healing.
Medication-Related Causes
Some medications can cause mouth ulcers as side effects, including:
-
non-steroidal anti-inflammatory drugs
-
certain antibiotics
-
chemotherapy drugs
Medication review is important in recurrent cases.
Smoking and Tobacco Use
Tobacco use damages oral tissues and reduces blood supply.
This:
-
slows healing
-
increases ulcer frequency
-
worsens pain
Quitting tobacco improves oral health significantly.
Infections and Systemic Conditions
Certain infections and systemic diseases may present with mouth ulcers.
Examples include:
-
viral infections
-
tuberculosis
-
autoimmune disorders
ICMR reports note oral ulcers as a common early sign in some systemic illnesses.
When Frequent Mouth Ulcers Need Medical Attention
Seek evaluation if ulcers:
-
recur frequently
-
last more than two weeks
-
are unusually large or painful
-
are associated with weight loss or fatigue
Persistent ulcers require investigation.
How Frequent Mouth Ulcers Are Diagnosed
Evaluation may include:
-
blood tests for deficiencies
-
assessment of gut health
-
immune screening
-
oral examination
Diagnosis focuses on identifying root causes.
Preventive Measures to Reduce Recurrence
Effective strategies include:
-
correcting vitamin deficiencies
-
managing stress
-
maintaining oral hygiene
-
avoiding trigger foods
Long-term prevention depends on addressing underlying factors.
Role of Preventive Health Checkups
Regular health checkups help detect:
-
anemia
-
vitamin deficiencies
-
metabolic issues
Early correction prevents recurrent ulcers.
Importance of Diet in Ulcer Prevention
A balanced diet rich in:
-
green leafy vegetables
-
fruits
-
whole grains
-
adequate protein
supports oral tissue repair and immunity.
Conclusion
The causes of frequent mouth ulcers often extend beyond the mouth itself. Nutritional deficiencies, stress, immune imbalance and digestive health issues are common underlying triggers. While occasional ulcers are harmless, frequent recurrence should not be ignored. Identifying and correcting root causes through proper nutrition, stress management and medical evaluation can significantly reduce ulcer frequency and improve overall health.
References
-
Indian Council of Medical Research (ICMR) – Micronutrient Deficiency and Oral Health Reports
-
National Family Health Survey (NFHS-5) – Nutrition and Anemia Data
-
World Health Organization (WHO) – Oral Health and Immune Function Guidelines
-
Lancet – Aphthous Ulcers and Systemic Health Studies
-
NITI Aayog – Nutrition and Preventive Health Reports
-
Statista – Oral Health and Nutritional Trends